A claim never arrives at a convenient time. It shows up after an accident, a medical emergency, or a loss that already has the customer stressed. What happens next decides everything. Not just the payout, but whether the customer trusts the insurer again.
Inside most insurance organisations, this moment still triggers a familiar chain reaction. Emails start flying. PDFs get downloaded, renamed, and re-uploaded. Adjusters open spreadsheets, cross-check policy details, and manually verify documents one by one.
What should be a straightforward process slowly turns into a bottleneck. Settlements drag on, decisions vary from case to case, and fraud often hides in plain sight.
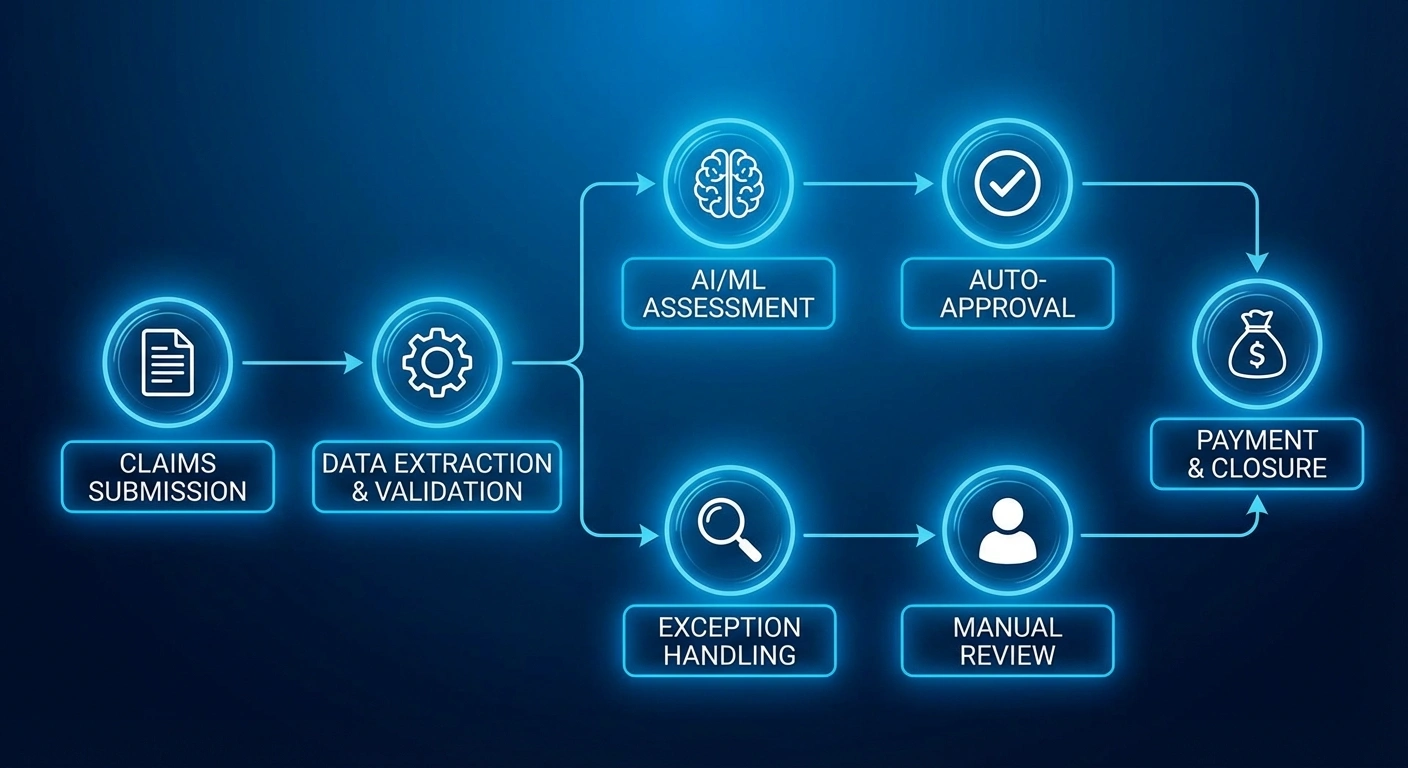
This is where Automated Claims Processing Insurance changes the story. Instead of treating claims as paperwork to be pushed through, insurers apply AI, OCR, and intelligent risk scoring to make claims smarter from the first second.
Documents get understood instantly, risks are evaluated in real time, and genuine claims move forward without unnecessary friction. The result is faster settlements, calmer customers, and automated insurance claims that finally work ahead of the problem, not behind it.



 16 mins
16 mins

